Brachial Plexus Nerve Block for Shoulder Surgery
This leaflet has been prepared by Ms. Delaney in collaboration with Dr. Justin Lane, consultant anaesthetist and pain specialist, with input from patients who have had a nerve block for shoulder surgery and using material from the Royal College of Anaesthetists (UK) patient information leaflet.
Please pay particular attention to the information in the section After Surgery.
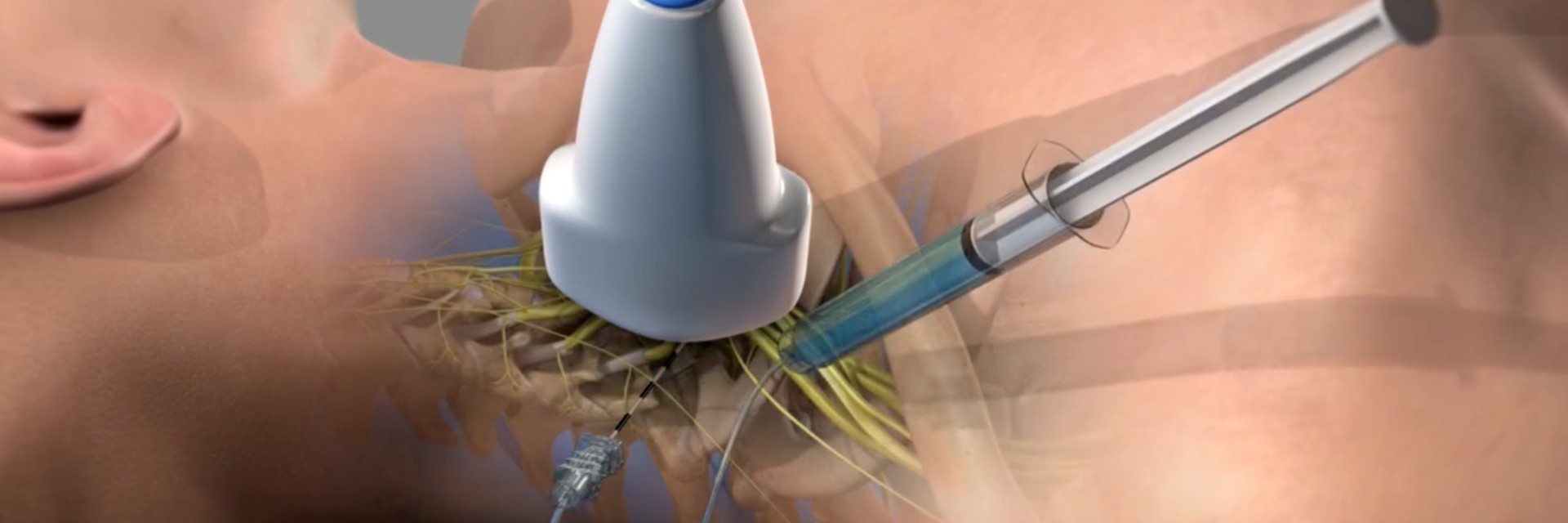
The brachial plexus is the network of nerve roots combining to form nerves that supply sensation and movement to the entire arm from shoulder to fingertips. A brachial plexus block is an injection of local anaesthetic around that group of nerves which temporarily blocks signals going through the nerves, including pain signals from the shoulder back to the brain. This can be helpful during and after shoulder surgery as it may lessen the amount of general anaesthetic drugs you need and therefore lessen the side effects of those, and it will also make the first night after surgery more comfortable. In certain cases, such as for capsular release for frozen shoulder, we use the window of complete pain relief provided by the block to start physiotherapy and get ahead of any potential for the shoulder to stiffen up again by having the physiotherapist stretch the shoulder immediately, while the block is keeping you comfortable.
Not all operations are suitable for nerve blocks and a nerve block may not be suitable for certain patients. The consultant anaesthetist taking care of you for your surgery will discuss the option of a nerve block with you if it is appropriate for your case and if the surgeon has requested it.
If you wish, you can be sedated when you have the nerve block injections or the nerve block can be performed after you are asleep under general anaesthesia. The anaesthetist will discuss with you which option is best for you.
We usually supplement the nerve block with a light general anaesthetic, because it can sometimes be difficult to sit still in the surgical position for the duration of your shoulder operation if you are awake with only the block providing regional anaesthesia.
The benefits of a brachial plexus nerve block include:
- Better pain relief after surgery
- Less need for strong pain killers, which can make you feel sick and may cause constipation or possibly have a risk of addiction if used for a long time
- Less need for a heavy dose general anaesthetic, which can lessen the side effects which include nausea/vomiting and prolonged drowsiness or tiredness
- Being able to get up and move around earlier after surgery and potentially leave hospital sooner
Before Surgery
You will have been given pre-operative instructions at the time of booking your surgery. It is important to note the instructions about fasting for a minimum of six hours before your procedure (to ensure an empty stomach and avoid the risk of food or liquid from your stomach coming up into your throat and lungs during your anaesthetic, which can be dangerous for you). It is also important that if you are taking any drugs to thin your blood that you let the surgeon and the pre-assessment team know which medication you are on so that a plan can be put in place as to whether you need to stop these drugs for a period of time before surgery or go on an alternative blood thinner temporarily around the time of your surgery. This may also need to be discussed with your GP and with any other prescribing doctor, for example a cardiologist if you have one, therefore it is important to let us know ahead of time.
Your anaesthetist will discuss the plan for your anaesthetic with you on the day of surgery and will explain the nerve block to you, if your case is appropriate for the option of a nerve block. You will have the opportunity to ask any questions at that time.
At the Time of Surgery
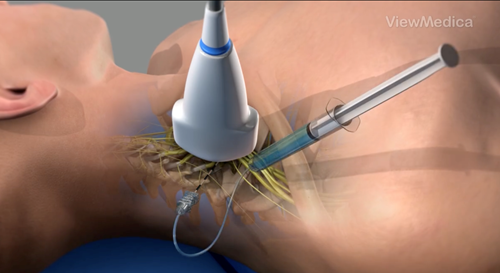
The nerve block will usually be done in a room near the operating theatre or it may be done in the operating theatre itself. The injection for a brachial plexus block is typically done in the side of your neck but additional injections may also be done close to your collar bone or shoulder blade or in your armpit. The skin is cleaned and some local anaesthetic is injected into the skin to numb it. The anaesthetist will then use either an ultrasound and/or a nerve stimulator which is a small machine that makes your arm muscles twitch to locate the nerves.
Most people find that the injection is no more painful than having an IV cannula placed or a blood sample taken. Your arm will start to feel warm and tingly and then heavy and numb. The injection can take 20 -40 minutes to start working, so in many cases you will go to sleep with your general anaesthetic before the arm is totally blocked and it is only when you wake up that you will experience the arm being numb and heavy. If you are given sedating medicine for the block or if the block is performed after you are first given the general anaesthetic drugs, you may not remember anything about receiving the nerve block injections.
After Surgery
If the block is working well, your entire arm from shoulder to fingertips will be “asleep” for the duration of the block, which can last up to 48 hours. Your arm will be numb and you will not be able to move any of the muscles. The sensation of not having any control over your arm and hand can be alarming but it is normal after the block and it is temporary. The nurses in the recovery room or on the ward may ask you to move your fingers in order to check whether your block is still in effect, this does not mean that they expect you to be able to move or feel, they are just checking to see if you are likely to need additional pain medication based on how well your block is working or not. You will need a sling to support the weight of your arm while the block is in effect.
While you cannot feel your arm and hand, take special care not to inadvertently injure yourself. Be particularly careful around heat sources such as fires or radiators or if using ice on your shoulder. You will not feel heat or cold while your block is working so pay attention not to burn yourself or cause cold injury to the skin.
Start taking your pain relief medication before the block wears off, as instructed. Do not wait until you feel pain to start taking pain relief as it can take time to then catch up and become comfortable. The block can sometimes wear off quite suddenly so it is important to get ahead of any potential pain.
When you start to feel some tingling or pins and needles and you start to regain some movement in your fingers, your block is starting to wear off and you should make sure that you have some pain relief on board as you will soon start to regain sensation in your shoulder after that.
If you are going to sleep for the night and you have still not regained sensation in the shoulder and therefore have no pain at all, which is very common the first night after surgery (and is a benefit as it helps you to get a good night’s sleep), make sure to take pain relief before going to sleep as it is possible that the block may wear off completely while you are asleep and if you have no pain relief on board, this may cause you to wake with pain that can be difficult to then control from a starting point of having no pain medicine in your system.
When to Seek Further Help
If you notice unexplained breathlessness or if your block has not fully worn off two days after the operation, you should contact your anaesthetist by calling the number given on your discharge paperwork.
Side Effects, Complications and Risks
Serious problems are uncommon but risk cannot be avoided completely. People vary in how they interpret words and numbers. This scale is provided to help.
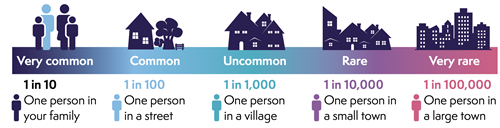
Anaesthetists take a lot of care to avoid all the risks given in this section. Your anaesthetist will be able to give you more information about any of these risks and about the precautions taken to avoid them.
Risks:
- Injection in the side of the neck: hoarse voice, droopy eyelid, changes in your vision and possibly some shortness of breath. These side effects are common and temporary. They go away as the block wears off.
- Injection around the collar bone: there is a rare risk, less than 1 in 1,000, of damage to the covering of the lung (the pleura) which can lead to some degree of collapse of the lung – called a pneumothorax. Air goes into the space between the chest wall and the lung, called the pleural space. Treatment depends on how much air gets into this space – it may cause no symptoms at all or if it is a large amount and you become short of breath, you may need a chest drain (a plastic tube) to help manage it.
- All injection sites: it is common for a small blood vessel to be punctured, your anaesthetist will put pressure over the area to stop any bleeding.
- There is a rare risk of having a seizure or another life-threatening event. Your anaesthetist will manage any of these situations if they arise promptly and expertly.
- Nerve damage:
- The risk of long term nerve damage caused by a brachial plexus block leading to altered or loss of sensation or power is difficult to measure precisely. Studies show that it happens in between 1 in 700 and 1 in 5,000 blocks – meaning it is uncommon or rare.
- Very commonly, about 1 in 10 patients notices a prolonged patch of numbness or tingling in their arm. These symptoms will resolve within six weeks in 95% of these patients, and within a year in 99% of patients.